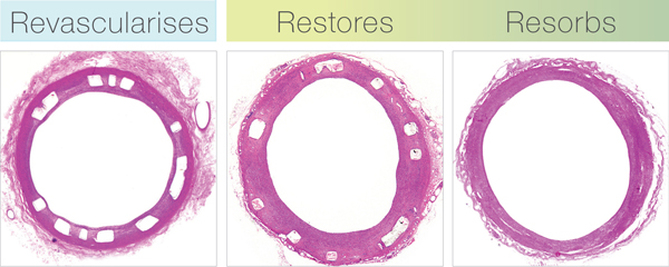
 The first coronary stent was implanted in 1986 by Dr Ulrich Sigwart. Stents are metal scaffolds which have revolutionised coronary angioplasty. Prior to stents, coronary dissection, caused by balloon angioplasty, usually resulted in an emergency coronary bypass operation or at best a 90% stenosis was reduced to a 40% one. Stents solved these problems but led to different ones. First there was stent thrombosis. Patients were initially treated with aspirin and warfarin to inhibit the clotting pathways but the bleeding problems were terrible. Then we then realised that aspirin could be combined with ticlopidine and subsequently clopidogrel to provide a safe treatment to reduce stent thrombosis but without the bleeding. Then there was the problem of restenosis (re-narrowing) at the site of the coronary stent implant. This led to spot stenting to keep the length of stent as short as possible. After that and thanks to Antonio Colombo and the use of intra-vascular ultrasound we realised that stents needed to be implanted at high to reduce restenosis. However problems with restenosis still existed and cardiologists developed complex treatments such as brachytherapy (intra-arterial radiotherapy) which now have all but disappeared. In the early 2000's we were introduced to the drug eluting stent. First Cypher, then Taxus and then the second generation stents such as Xience, Promus and Integrity Resolute. No longer did interventional cardiologists have to worry about the length of stent they were implanting. Treat from normal vessel to normal vessel became the mantra. But the downside was stent thrombosis, originally thought to just be a short term problem it is clear that it could occur years after stent implantation. Also in some high risk patients such as those with diabetes the restenosis problem has not been completely solved. There are some patients with in-stent, in-stent re-stenosis for which the treatment options are limited. The holy grail of stenting has been seen as the biodegradable or resorbable stent. Implant the stent when it is needed for the first few months and then when it has done its job, like a self absorbing suture, it dissolves away. This sounds an attractive prospect and in 2012 the world of stenting was revolutionised by the entry of the first commercially available biodegradable stent called ABSORB. In the early phase after implantation the ABSORB revascularises like a drug eluting stent. It releases the anti-proliferative drug everolimus to minimise neo-intimal growth and restenosis. During the restoration the scaffold benignly resorbs and the stent gradually ceases to provide luminal support resulting in a discontinuous structure embedded within the coronary artery. As the scaffold degrades, the polymer is converted into lactic acid which is metabolised and is ultimately converted into benign by-products of carbon dioxide and water. Several studies support this concept and indicate that there is no clinical benefit of a permanent stent over time. The ABSORB eliminates the permanent mechanical restraint on the vessel and should allow for more normal blood vessel function. Three-year results from 101 patients in the second stage of the ABSORB trial have shown that the rate of major adverse cardiovascular events was 10% at three years, similar to a comparative set of data with a best-in-class drug eluting stent at the same follow-up period. In a subset of 45 patients, intravascular imaging techniques showed improvements in vessel movement and a 7.2% increase in late lumen gain (an increase in the area within the blood vessel) from measurements taken at one and three years. These findings are unique to the absorbable stent and are not typically observed with metallic stents that cage the vessel. The ABSORB stent is now available and patients interested in receiving it should discuss with their cardiologist to see if they are suitable for the device. References: ABSORB II Trial ABSORB-Extend Trial
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
Dr Richard BogleThe opinions expressed in this blog are strictly those of the author and should not be construed as the opinion or policy of my employers nor recommendations for your care or anyone else's. Always seek professional guidance instead. Archives
August 2023
Categories
All
|
||||||
 RSS Feed
RSS Feed

