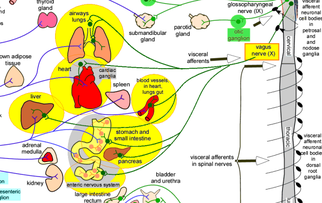
 When doctors are asked to classify atrial fibrillation (AF) they usually start by describing it as paroxysmal (coming and going) or persistent. When they are asked about the causes of AF they will usually list high blood pressure, ischaemic and valvular heart disease, alcohol and over active thyroid. These things are definitely associated with AF but what triggers episodes. Another way of classifying AF is Sympathetic or adrenergic AF and vagal AF. The initiator of the AF episodes can often be overlooked in the consultation but is very important particularly as vagal AF will gets worse when treated with beta blockers. The vagus nerve wanders from the brainstem throughout the chest and abdomen innervating the heart, lungs and intestines. It is part of the autonomic nervous system and its cardiac action is to slow the heart. For some patients increased vagal activity is associated with the initiation of atrial fibrillation. So called vagal AF is enigmatic but should be more recognised. This is important because it needs to be managed differently from other more common types of atrial fibrillation. When to suspect vagal AF: If the arrhythmia occurs at rest, after meals or during sleep then it is more likely to be vagal stimulated. Commonly this type of AF stops in the morning or during periods of exercise and can be precipitated by cough, nausea, after eating, swallowing and ingestion of cold foods and drinks. Vagal AF is more frequently seen in younger patients (30-50 years old), typically men and usually the heart is structurally normal on echocardiography. If the patient participates in endurance sports such as cycling, marathon running or cross country skiing then AF is also more common. ECG recordings often show a combination of atrial flutter alternating with atrial fibrillation. When a 24h ECG monitor is performed sinus bradycardia usually occurs before the onset of the AF. The ventricular rate during the AF is generally not fast. It is possible to measure the activity of the autonomic nervous system but it is difficult. One way is to assess heart rate variability which can assess the balance between the sympathetic and parasympathetic or vagal tone. Vagal stimulation shortens atrial effective refractory period and augments the ability of a single atrial premature beats to induce AF. How should vagal AF be managed? Anticoagulation as per the underlying stroke risk predicted by CHAD2VASC score should be considered. With respect to reducing vagal AF episodes there are only anecdotal data about the best way to manage this. Drugs which block the sympathetic nervous system commonly used in the management of AF such as beta blockers and digoxin should be avoided. Alternative drugs such as those which reduce vagal tone should theoretically be effective. These drugs include flecainide, quinidine, and disopyramide. The pulmonary veins are a well-recognised source of AF in many patients and ablation can be effective in reducing paroxysmal AF. In contrast there are no specific studies reporting the success of ablation in vagal AF. One recent development is the awareness of increased activity of the If channels which raises the possibility that blockade of these channels with ivabradine might have an anti-arrhythmic in vagal AF patients. This is still an area for research and further information will be needed before this can be used routinely in the clinic.
100 Comments
Serge
7/5/2017 06:03:03 pm
Interesting article. I'm 41, diagnosed with AF when I was 32. Normal echo and stress test. I typically have 1 to 5 AF episodes per year lasting 2 to 10 hrs with spontaneous conversion to NSR. Episodes only happen at night. AF ventricular rate is always <100 bpm, usually about 80 bpm. NSR resting rate is 50-60 bpm, but has been measured in the 40s. I'm currently not taking any medication although I do have a prescription for flecanide pill-in-pocket, which I have never taken. I'm an avid cyclist and cross-country skier and participate in other sports. I seem to always have more episodes during the winter. I have an episode in the first week on January every year. I have long wondered if this was related to xc skiing. Cardio + cold weather? Is participating in endurance sports contra-indicated for people with Vagal AF? Thanks.
Reply
jeffrey armbruster
8/11/2017 09:21:11 am
Yeah I was an avid nordic skier too. My first episode occurred immediately after I skied hard for three days (felt great!) There's plenty of evidence that people who engage in high aerobic activity sports are prone to afib. That certainly fit me. You might consider switching to downhill or perhaps leisurely skiing through a flat forest. And check your heart rate while Nordic skiing--I was astonished at how high mine went! (I skied at altitude though). Good luck!
Reply
RJ
28/1/2018 10:33:54 am
I too have paroxysmal Afib. Active 48 years with perfect blood pressure, perfect cholesterol and no diabetes. Engage in strength training yoga, and now walking only (no running) Afib occurs about 1-2 times a year since 2011 always in January or February where it is prolonged enough to visit ER with spontaneous conversion or with meds. First several short episodes happened in my 20s but never during exercise. Never drank, smoked or nothing else. Don’t do caffeine or alcohol and avoid medications that are stimulants or depressants. Clean living. Only complication is exposure to 9/11 and must where Cpap despite ideal weight and BMI.
Reply
Greg
17/6/2017 02:12:44 am
Very interesting and a dilemma! I am 39 - have tachycardia episodes once every 3-8 months for 10+ years - they are always brought on by either bending over (most common), sitting on toilet, and once by jumping into cold weather. I also get ectopics slouching and after eating beans or spicy food sometimes. I was convinced these tachycardia episodes were more common SVT episodes until I finally caught one on EKG last week and the reading came back as Atrial Flutter. My issue is that I know my triggers and all of these seem to increase vagal tone - also, it seems that before going into tachycardia I have 5-15 seconds of heart beating very irregular but not as rapid. Then it is either rapid and irregular or just rapid and regular (clocked it twice at 160, in ER was 147-153 sustained). The dilemma! Sounds like vagal A-fib is not fast and also happens mostly at night - mine is fast and happens mostly in daytime. I have heard that vagal A-fib can organize into Aflutter... would that flutter also not be fast and always be at 4:1 ratio or could it be fast and at 2:1 conduction? My big fear is reading contraindications on these medicines and getting the wrong one in ER and getting pushed into 1:1 conduction of A-flutter or being given beta-blockers or adenosine inappropriately. Have no clue what to do but I know they are treating this as typical Atrial flutter at this point yet they did not ask me about triggers and they all seem to be vagal... and vagal maneuvers have tended to stop episodes in past... not even sure if you are out there and respond but I really appreciate your writing and any thoughts would be helpful!
Reply
David
22/6/2017 12:31:51 am
I've had vagus nerve response A-Fib since 1992. It is currently 2017. They tried flecanide, and other drugs that you mentioned and they did not work. You mention that Beta Blockers do not work, but Sotalol works for me. I do have episodes, but they last one or two hours (most times just a couple of minutes) and they happen about once every four or five years.
Reply
Serge
22/6/2017 05:00:06 pm
Hi David. You have described my experience with afib exactly: the connection to gastro, the low-normal potassium, sleeping on left side aggravation and relief from inclined thorax. In light of our similarities, a few questions for you if you don't mind.
Reply
Carol
3/7/2017 10:45:50 am
Reply
HayUK
21/7/2017 09:08:46 am
Dr Bogle, most interesting about beta blockers not helping Vagal AFib. I had to decline bb's cos (1) I'm asthmatic; (2) my BP has always been in normal range. I've had Persistent AFib for 21 years (since age 36 yrs) due to an accident whereby C5/6 spinal disc prolapsed, Rt TMJ (jaw) joint dislocated, ditto Rt shoulder. Is it possible Vagus Nerve function impeded, causing Persistent AFib, main symptom of which is extreme giddiness upon straightening from 5 seconds bending down (tying shoelace) or 3 mins (weeding garden). Also (1-2 per month) get migraines with projectile vomiting (often undigested meat+veg dinner from previous evening) & full bowel incontinence.
Reply
Daniel L Mask
29/8/2017 11:45:29 am
You suggest Ivabradine...The research shows that Ivabradine (Corlanor) CAUSES a fib.
Reply
Blaine
13/9/2017 06:27:28 pm
I had to pick my jaw up off the floor after reading this. For 9 months I have been trying to get my cardiologist to listen to me. My AFIB actually started a couple of days after a slip and fall that tore my rotator cuff. It seems I also injured my back between T3 and T5. Muscles knot up in this area and the more they are aggravated the more often I have flutter that will go into a full attack if I don't stand up and straighten my back. In addition, I found that taken the prescribed beta blockers may be affecting the number of attacks I have. I recently quit taking them and started improving. Additionally, my back doctor gave me a steroid shot in the muscles in spasm and after 2 days I battled with flutter and AFIB nearly every waking moment. Been about 3 weeks and I am starting to improve now as the injection wears off. Lying on my left side will trigger an attack. Poor posture, (slightly slumped over while sitting) will trigger and AFIB attack. For whatever reason, laying back in my recliner will trigger an attack. Most recently, eating is now triggering attacks. My full blown attacks come mostly while I am asleep because I roll over on my left side. They wake me up and I have to go on a 30 minute power walk to get the heart back in rhythm. I have told all of this to my cardiologist who simply looks at me like I'm stupid and tells me they don't really know what causes AFIB. I have known what causes mine from day one and this article best describes it. I will bring up vagal Afib to my cardiologist and if he choses to blow me off again, I will find someone in my area that is wilingl to work the cause.....Thank you so much for posting this. I feel I have a renewed chance to rid myself of this.
Reply
Nancy Bates
17/7/2019 09:12:45 pm
My symptoms match what others are stating. I wanted to add that I started adding ‘humming’ out loud since it was used for Vagal issues in some other programs and it WORKED - I’ve used it four times now, and it has converted my heart each time...
Reply
Joann
15/9/2017 06:45:24 am
After reading all this I know I have vagal afib, and have most all the symtons that everyone reported! The dr has me on a beta blocker and the fibbing is getting worse! Every time I get ready to go to bed I start fibbing, last night 6 hours! Does anyone know what is a safe blood pressure medication that won't cause more afib?
Reply
Vicki
6/8/2019 10:39:39 am
I've had Afib on occasion but discovered via hair mineral analysis that I was actually low in calcium, potassium, AND magnesium - all which can contribute to arrhythmias if not kept in balance. Blood work still 'appeared' normal, however. Since addressing this, I've been fine, but I match all the criteria of vagal AF because mine has always happened after midnight. Magnesium dips low at that time since it has a diurnal rhythm, so I now make sure I don't skip my evening dose. Stress depletes magnesium in particular but all our minerals go haywire under stress. The blood tests may look in range but the body keeps blood tightly regulated - and that doesn't necessarily show what's in the cell.
Reply
John Bedson
24/10/2019 03:16:34 am
Joann: Try Verapamil. Vagal afibbers should never use beta blockers. Verapamil is good with vagal afib.
Reply
HTForb
25/9/2017 04:45:04 am
I was diagnosed with AFib at 48, female, healthy bmi. Medication made AFib worse and I knew there was a vagus nerve connection because I could feel constriction in my abdomen before AFib. Went on the FODMAP diet (Stanford created it - google it) and then slowly began introducing foods back to see if it triggered AFib. Found 2 culprits: gluten and caffeine (specifically coffee). In last 3 months since eliminating these had one bout of AFib - and that was when I tried gluten again. They say coffee is ok for AFib - not for me. Happy to be AFib free and off medication.
Reply
Wendy
27/9/2017 09:39:01 am
I have been experiencing what I believe is also vagal afib. I get it multiple times a night, nearly always when I am sleeping on my left side and sometimes when laying on my back. I wake up in a panic and feel like I'm having an anxiety attack. I feel like I need a pace maker. In order to make it stop I take a deep breath and hold it for a few seconds. Sometimes I have to do it a couple of times but then you can feel your heart beat go back to normal. I'm not overly active but I do like to have a glass of wine at night. I take a lot of medications for migraines. I wonder if any of these are contributing to the afibs or if the afibs are contributing to the migraines? I mentioned it to my doctor but she didn't seem concerned. I am in my early 50's but my family has a history of strokes and this might be why.
Reply
Marita Hensel
30/4/2018 05:38:06 am
My Afib is definitely triggered by even a few sips of wine. Of my last four one I had a glass of wine with dinner.Two, has 3 sips of wine on Christmas eve. Three had a ice cold glass of juice, and 4 had a snack before bed. The only afib which happened immediately was after the ice cold drink, The others are always 2 - 4 hours after and can last anywhere from 1 hour to up to 10 hours. I do take an Eliquis to prevent clotting when I have a bout.Also am on Cardizem and take an additional cardizem to stop the afib, sometimes it works quickly sometimes not, but it does keep the pulse rate within reason. Learning all the things that trigger it. Caffeine, gluten, alcohol, ice cold drinks, cold meds and eating before bed.
Reply
Eric
31/7/2018 01:21:51 pm
Hi Wendy,
Reply
rickycz
1/10/2019 09:03:24 am
try to eliminate food and drink high in Tyramine. Wine has lots of it as do others foods and beverages. Tyramine is also linked to migraines.
Reply
Terry
12/10/2017 06:06:47 pm
I suffered the same afib scenario for about a year. I am 59 160lbs. I have not had an episode of afib now for about two years. I found most of my relief by taking a magnesium supplement and applying magnesium oil (ancient minerals) every day. I have the “pill” but have only used one in two years. I am going to try giving blood this week to see if that makes me feel more comfortable internally. I will let you all know if it helps with anything.
Reply
Terry (update)
14/12/2017 07:21:28 pm
I started taking magnesium taurate (500 mg/day) and 1000mg of taurine per day and am very happy with the results. Am feeling a lot less anxious and afib/palp. free. Also stomach is more “comfortable”. Both magnesium and taurine are considered safe and natural so try it !
Reply
Mike
18/10/2017 01:37:33 pm
I only discovered this website today after I had a consultation with a cardiology pre-assessment nurse prior to my ablation operation schedued for 23 October. She mention the relationsip of the vagus nerve with Afib. So here I am after Googling “afib and vagus nerve”.
Reply
Mark
13/11/2017 03:16:22 pm
I'm so glad to have found this webpage, and the comments left by others. I am convinced I have vagal afib. I have had afib episodes over the last 20 years, sometimes years without having one, though.
Reply
Douglas
13/12/2017 06:29:23 pm
I got afib for the first time about 8 years ago while helicopter skiing. I am sure it was initially brought on by fear and anxiousness however my father had it so there is I am sure a genetic link. It occurred at night, would not revert until I worked out for 15 minutes or so getting my heart rate up and this went on for 4 months. I did a lot of research and found a link where a survey was done of thousands of affibers for the effect on their afib of natural supplements they were taking.Of all the responses the overwhelming most positive was Taurine which is naturally occurring in the human body. I started taking 3000 mgs per day and within a month my afib was gone. In the past 8 years it has come back only once, when I got a steroid shot a couple of years ago. It lasted about 50 hours and I upped by intake of Taurine to 5000 mg. It has never come back.
Reply
Alan Hill
14/12/2017 06:35:10 am
3000 mg of Magnesium Taurine ?
Reply
michael
15/3/2018 10:55:09 pm
I just read your post and got chills... I was first awakened by "the beast" at 3am. one night, almost three years ago. I played golf that day--it was a little warm and I did not have enough water, and I flew home from a long trip the day before--and had a couple (2) of glasses of wine with dinner and went to bed. I chose to go to the emergency that night, because...well, I was frickin scared. I had never experienced something like that before...
Reply
Jeff
5/4/2018 10:13:07 am
Michael thank you for sharing your story. I have had your exact experience and learned dehydration can cause incidents for me too (I don't drink alcohol at all out of fear of that). Is there a particular electrolyte solution you like? I have found electrolyte water, but the packet sounds portable.
Jeff
5/4/2018 10:10:04 am
Douglas this was very helpful. Do you happen to recall the location of the survey that you found? It sounds great. Congrats on your success with increased Taurine, I am going to ask my functional medicine Dr about increasing my dosage from 500mg/day.
Reply
Michael Crabb
6/4/2018 09:04:46 am
Yes, Jeff! It's a product called Ultima. You can order it from Amazon or pick it up at Wholefoods. They are so convenient and I take them everywhere. I also take Taurine, Arginine, and L-Ribose three times a day; along with Amazing Grass/Green Superfood/Berry Flavor. It has all of the antioxidants i need. let me know if there is anything else that I could suggest and you do the same.
Andrea Picazo
17/10/2018 09:12:06 am
Hello,
Reply
Vic Merrill
31/7/2019 11:43:58 am
I would Really like to know how you’re doing now. Today’s date as a reference is July 31, 2019. Would really love to hear from you as your situation is almost identical to mine. Thank you
Reply
Bev
7/1/2018 12:49:42 am
My AFib attacks, 5 since 2008, have every single time been the result of vomiting. 4 were from migraine, last one from something I ate. Ive tried taking ginger gravols a lot when any slight feeling of nausea arises, as has been happening the last month or 2, and the hospital (I have to be cardio- verted each time) even gave me some pills they give chemo patients for nausea, which didnt work this last episode a few days ago. So they are thinking my AFib is caused by the Vagus nerve. How to fix that I do not know. Theyve just opened an AFib clinic in town, which Ive been referred to. Anyone else heard of vomiting causing AFib? How can that be fixed? My attacks are getting more frequent.
Reply
Richard
7/2/2018 02:47:59 pm
It has been almost 4 years since Dr Bogle posted this extremely helpful, interesting piece. I most definitely have paroxysmal vagal AF. I suffer a 12-18 hour duration A-Fib episode roughly every 2-3 weeks. I am on Flecainide 100 mg B.I.D., Apixaban 5 mg B.I.D. and Metoprolol (beta blocker) 25 mg B.I.D. A few days ago I decided to reduce my Metoprolol dose by half, with the intention of completely eliminating Metoprolol from my drug regime within the next 2-4 weeks. I've read several articles now that say beta blockers are contraindicated for people who suffer with vagal AF.
Reply
June
14/2/2018 06:13:54 am
I am a 62 year old woman and started with AF in July 2014 after a strenuous Zumba class. I had also been taking a medication for blood pressure for only 3 days. The AF started in bed (2am). It woke me with a start! I thought I was dying! I had taken Sotalol 80mg daily for over 20 years after suffering palpitations in my 30's and it had always worked well, but after the first AF episode it seemed to stop working. To cut a long story short I now take a combination of 50mg Flecainide and 1.25 mg of Bisoprolol morning and evening but still suffer AF episodes lasting between 3 and 12 hours, almost always during the night or early morning if I have to get up to go to the bathroom. I can't lay on my left side or my back in bed and still don't know the triggers for my episodes. I cut out caffeine and alcohol back in 2014 and am now frightened to exercise. I still get palpitations too. Just for info the cardiologist prescribed Warfarin because of the increased risk of stroke, but in 2016 I suffered a brain hemorrhage so now refuse to take it. I will try Taurine as I am at my wits end - the only thing the cardiologist recommends for me now is ablation and I am worried that won't work either. I used to be so healthy, doing zumba, aerobics and running but now feel I can't do anything except wait for the next episode!
Reply
Elizabeth Kirk
9/3/2018 05:55:44 pm
Most of these symptoms fit me... just had a complete GI workup done because of the nausea. nighttime problems, sleep problems, massive hiatal hernia which I felt was involved, etc.. Have been talking to a chiropractor who is working with me also about vagal possibilty. He is currently reading info I gave him... This blog totally confirms my suspicions, but now the main question for any of you, is: How do you get your cardiologist to listen to what you say when you describe these syptoms over and over and over ,and they act like you are nuts? What treatments have YOU found helpful. I see magnesium andd Taurine, ,etc. i have changed all eting patterns, already sleep in semi sitting position. Used ice previously to stop episodes and it worked.. Help please... Main question, how did you get your cardiologist to work with and understand your problems. I am on my second one.. first wanted to do immedaite ablation procedures, etc. and a pacemaker was placed after a total blockage.
Reply
Matt
28/3/2018 06:41:03 pm
This is stunning. I was diagnosed with AF when I was 26. I am now 34 and have had two ablation surgeries with about 80% success. I am on a combination of flecainide and ditalizem daily to manage symptoms.
Reply
michael
29/3/2018 08:16:40 am
Hi Matt. Read this article.(http://www.drdalepeterson.com/Arrhythmias_dffd837f.html) Buy these three little miracles.! It's three simple amino acids! They don't make the all-in-one powder anymore because the three amino acids don't live together (in a jar) very well--they stick together. HOWEVER, I bought the three separately (L-Taurine, L-Arginine, and D-Ribose powder and started taking the suggested amounts three times a day. WOW! I have not had one flutter (seriously!)since I've been taking this simple amino combination. And, my heart rate is around 82 when I wake up in the morning these days; It used to always be around 100 and with flutters. You can get these at Wholefoods or a vitamin store...H-o-n-e-s-t-l-y...try this--it works!
Reply
Jeff
5/4/2018 10:20:14 am
In light of how expensive ablations and ER visits are, I am eternally amazed how lazy the medical profession is about figuring out how to fix our problem. It's been great reading everyone's comments here, I feel like I have found my people.
Reply
Michael Crabb
6/4/2018 09:09:15 am
Hey Jeff. Me again. I too spent a lot of money getting blood test for electrolytes; I even spent extra for the intracellular test. Everything was normal, but that does not explain why I benefit for electrolyte solution a couple of time a day as needed. Even if your test come back NORMAL, I would do the electrolyte and the Taurine, Arginine, and L-Ribose anyway. I think it makes a HUGE difference...
Reply
Dan
4/6/2018 12:57:57 pm
Jeff, it turns out that coconut water has far more potassium than bananas. It also has some antifungal, antiviral and antimicrobial properties.
Reply
This has been interesting reading all the comments about this vagal afib. For me I just had open heart surgery to correct the afib by having a Cox 4 Maze ablation and a mitral valve repair. What brought on a lot of the symptoms that are so unique that my PC wants me to write a paper to submit to the journal of American Medicine about the fact that vagal afib is often precipitated with excess stomach acid. I have found that a regular regiment of Ranitadine helps in the reduction of stomach acid so that the vagal nerve does not get inflamed or irritated from the gastrointestinal system which brings on the paradoxical afib. I've had Endoscopies, Colonoscopies, CT scans and I found that the Ranitidine seems to be the only cure and resolution for the upset stomach which reduces the onset of the AFib.
Reply
Joel
9/4/2018 03:16:12 pm
I just wanted to reach out and say thank you to everyone. These posts have been a glimmer of hope. I am 35 and was just diagnosed with A-Fib. My CHARS score is zero and my echo and stress test were all good. I have been exercising 15-20 hours a week for about a year or so and just within the last few weeks have been in A-Fib. I went into NSR for a couple days, but then popped back into A-Fib after an intense workout. My HR has spiked up to upwards of 190 while resting when my normal resting rate is around 55.
Reply
Jessica
10/4/2018 10:26:20 pm
Wow!
Reply
Richard
11/4/2018 08:52:15 am
Hi Jessica,
Reply
Andrea Picazo
17/10/2018 09:48:44 am
Hello,
Reply
I think I could cry - ive had the worst time with racing pulse for no reason over the last 2 months - my gp/cardiologist/rhuematologist dont know whats causing it.... sitting still resting pulse can be 55-65 then minutes later pounding in my ears and its off to 100... seems to happen 1-2 hours after eating or if sit in a hunched posture......seeing neurologist next week as a sympathetic gp agrees its not anxiety and could be this - had blood tests for celiacs etc which so far have proved negative....
Reply
Nick Toth
22/4/2018 12:35:33 pm
Hi!
Reply
Sherri
23/4/2018 04:10:14 pm
Have had 4 episodes
Reply
I'm 38 yrs old, recently diagnosed with Afib, no thyroid problems or diabetes, no heart disease, no family history that I'm aware but I did have a car accident, sort treatment with a chiropractor and started having what I now know as Afib episodes. I suspected it was some how connected to my treatment and also thought possible dehydration and that was just a gut feeling not Dr's knowledge. One morning 5am getting out of bed to pee I had an episode that didn't fix itself and ended up in emergency. Tests galore where done, all negative, I was put on medications which didn't stop it and it was paddle shocked back to normal rhythm. I notice the worse my discs and neck problems are the more often I get episodes, only usually lasting 10 or so seconds, medications seem to return my heart back to normal rate, if I kink my neck for any period of time i.e. leaning head on my hand laying on my side can trigger episode and when I lay straight it stops. Before my hospital stay, I noticed I'd have an short episode if I sat in a chair and leaned a fair way forward (bad posture) to play on my phone at low desk etc would cause an episode, at the time I wondered did I cut off my own breath to cause it but now believe it was discs in my back or my chest somehow. I'm absolutely devastated by this happening to me, feeling extremely depressed because of it. I asked my chiro but of coarse she fobbed it off. Reading this article aswell as other research has made me feel stronger about vagus nerve being at least a major part of the cause :( Thank you for sharing everybody
Reply
Andrei
13/5/2018 10:16:47 am
Thanks a lot for this information. No I am going to inform my doctor about my diagnosis. I have AFb attacks at night time after I exercise
Reply
Diane
14/5/2018 04:36:59 pm
I’ve had very brief episodes occasionally over the years that I thought were caffeine-related & that I could stop with a cough or 2. But 7 years ago I had an episode that wouldn’t stop & I went to the ER. I’ve been on Sotalol ever since but still average an Afib episode about every couple of weeks. The majority of my episodes occur when I’m sleeping. I too have stopped alcohol & caffeine. I sleep on my right side because the left side is a trigger. Bending over or tight clothing at my waist are triggers, as are large meals especially later in the evening. I also feel too much sodium can be a trigger too. I too find that cardiologists seem apathetic about trying to figure out what can control vagal Afib. They routinely push for ablation but my feeling is that isn’t addressing the root cause. I’m grateful for this article & comments! First time I’ve encountered others with similar triggers.
Reply
Steven
15/5/2018 05:15:30 pm
I'm 37 male had first afib episode in August 2017 which woke me up at 2am. I think mine is vagal. But rather than having an episode after big meal, at rest or bending down, etc, mine only strictly happened when I was sleeping. I've tried everything possible but they didn't make any difference, only sleeping is the time that it happens. Anyone like me?
Reply
Steven Krupinski
19/5/2018 01:19:11 pm
Perhaps you have sleep apnea which is the trigger at night
Reply
LeeAnne
16/8/2019 05:12:23 am
Yes. I am undiagnosed, but have had many frightening wake ups about an hour after falling asleep. Rapid heart rate that wakes me, but slows after about 60 seconds. Scariest thing ever.
Reply
17/5/2018 07:24:04 pm
Wow! I have found my tribe and my afib home!! I have always “known” mine was vagus related and even in the hospital when first diagnosed asked several times about the distress I always feel in my abdomen during episodes. No credence given to it at all and vagus not even mentioned! They even did a Cat scan and just said I had a few small gallstones. UNbelievable. No wonder none of the drugs have given me any relief! I read The Magnesium Miracle early on and have been supplementing with it but it wasn’t until I got off the “standard” afib drugs that I REALLY started feeling better using the minerals, Tranquility, Heart Calm (mag taurate, potassium, taurine & coq10) and a few essential oils! This is shameful IMO.
Reply
Diane
18/5/2018 08:20:43 am
Hi Christine, I’m interested in a more natural path to dealing with my vagal Afib & wondered if you can elaborate on the essential oils you use.
Reply
Faith Bowe
16/10/2018 08:34:21 am
I just got diagnosed with parox. Afib about 2 months ago. I can’t believe what I’m reading here!!!! This is me to a tee! I’ve told my cardiologist these exact symptoms and she looks at me like I’m crazy. I asked her why I have so many attacks when I lay down and wake up with afib episodes. She says it’s because I’m quiet and notice it more. I call B.S. on that! I know I have nothing that feels like THAT during the day! You mentioned Heart Calm in your post. Is that something I can buy at a store or on the interments? Does it contain all those products you listed? I really want to try it! Thanks!
Reply
Gary Hopkins
2/9/2019 05:42:24 am
Wow, so glad to hear you say you have the distress in your abdomen as I also get the same feeling and always get shut down at the Dr's when I mention it. I also find that pushing on that spot can make me feel better and stop the Afib. How are you going with the supplements?
Reply
Bob G
22/9/2019 07:00:05 pm
What was the best regiment that worked in your case? I've taken Heart Calm, ylang ylang and aroma life (essential oils). But, that's it. I'd like to know what works for you. Thanks!
Reply
Bill
21/5/2018 12:20:31 pm
Vagal AFIB. I have had 18 episodes in the previous 14 months. These average around 6 days. Recently, one lasted 15 days. I have provided my main cardiologist with graphs showing these last 18 episodes with a date and a duration. He offered no observations on the data. In the last week I obtained a second opinion from an independent cardiologist. Except, he is really an EP. He did mention the Vegal AFIB, but was first recommending Cryo-Ablation.
Reply
sallie Goldberg
23/5/2018 10:15:59 am
I am very interesting in learning all I can
Reply
John
30/5/2018 09:27:39 am
Im not sure if I have vagal afib. Ive had 3 - 5 episodes since September 2016. The first was at 3 or 4am, I woke up to urinate, everything started spinning, I started sweating profusely, and instantly was zapped of every ounce of energy I had. I went to the ER and was told I was in afib. From what Ive read here, beta blockers, (Im on metroprolol and sotolol, as well as procardia, lisinopril, eloquis), dont work if its vagal. I think vagal because I noticed if was usually when I am full, in the evening, and food doesnt actually trigger it, but it feels like its trying to, and left side sleeping, and a pain on my left side, at the bottom of my rib cage, and I had gastic sleeve surgery November 2015. So I was put on eloquis, lisinopril, metropolol, but still kept having these episodes I call them, light headedness, sweat, high heart rate, and going into afib. Are these the type of things that happen when going into afib? I just want to make sure thats what it is. But they added procardia, and sotolol, and although I havent had an episode since they added the last med, sotolol, I sometimes feel like its trying to rear its ugly head. I get ectremely warm, and a touch lightheaded, but then it goes away. So for me, the triggers seem vagal, but the beta blockers are what helps. Wierd I guess.
Reply
Diane
30/5/2018 03:45:05 pm
Hi John, My triggers are similar. My symptoms are not as far as the sweating & lightheadedness, but I do have the rapid heartbeat & my heart feels more like a flopping fish as it beats irregularly. My bpm stay around 105 during an episode & I’m on Sotalol. I experienced 170 bpm during the pre-Sotalol episode that led to an ER visit. I’ve read that some people have a hybrid version of Afib, part Vagal & part Lone Afib. If you have a smart phone it’s helpful to get an App that tracks your bpm so you can tell your cardiologist more about your episodes. Maybe someday soon the medical community will have a better understanding of how to treat Vagal Afib.
Reply
John
1/6/2018 09:13:38 am
Hi Diane, I have the Kardia device as well as the Apple watch which tracks your heart rate. The first episode I had back in Sept 2016; when I went to the ER they said to me "Is your heart rate always in the 30's?". But every episode since, my HR has been high, last one being 190-something. The time before that my blood pressure was 288 over 212 but my heart rate was slow and the paramedic told me I was in afib but very slow heart rate. When I got to the ER they said I wasnt in afib. Im really confused, and just wonder if theres an underlying problem. I had a echo and they said my heart was slightly enlarged which doesnt surprise me because I used to run 10 miles a day and work out like crazy. When I hear about the symptoms people get when going into afib, most dont mention sweating or light headedness. Its terrible when it happens to me. I mean sweat like a bull and feel like Im going to faint. I have to shake my head from side to side to get out of it. Its terrible.
Rebecca
8/8/2019 01:57:33 pm
John, I know this long after the fact, but I wanted to tell you that the sweating, spinning, elevated heart rate, etc. could be dumping syndrome from having the gastric sleeve. When you have these episodes, do you usually have to have abdominal cramps and a bowel movement along with them? If so, it is probably dumping syndrome and that could be a trigger for your AF.
Reply
Dan
4/6/2018 12:53:33 pm
Male. 49 years. Heart otherwise normal, they say.
Reply
david samuels
26/6/2018 06:08:46 am
I am an anesthesiologist who is helping my friend who has all the signs and symptoms you describe for vagal atrial fibrillation. (nighttime events, after large meal, sleeping on left side) I wonder if there is any benefit from taking glycopyrrolate prior to bed to block the vagal effects on the heart.?
Reply
David
28/6/2018 10:42:49 am
I have been going through this for over 5 years now. I may have had the beginning of AFIB a lot earlier and didn't realized it. My whole process has been a long road and I am glad to find this site and especially the comments.
Reply
Ulysses G.
3/7/2018 10:47:45 am
Folks, I am beginning to think that mine is also vagal AF and something really is triggering my AF. My AF was detected in 2017 when I had my random annual checkup. I didn't feel any palpitation and my heart bpm was normal. Went into cardioversion, with no medication and it came back 5 months after. It came back when I had a very bad stomach flu. I knew it came back because I felt the palpitation this time. My cardiologist put me on propafenone at 300 mg x 2 but the medication did not help. Went into cardioversion again last week and still on medication. My cardiologist knew that I hate medication and promised to take me off the med if he feels its the right time. Currently there is no side effect except my normal HR went down 10bpm. I am hoping to get off the medication as soon as possible. I have been reading people taking all kinds of supplements here such as Magnesium, Taurine, COQ10, etc. I would so much prefer to take these supplements instead of Propafenone.
Reply
Sabina
3/7/2018 02:30:07 pm
Hello everyone, I had AFIB last 12 years. With my own research Ihave tried many different supplements and I had few different naturopathic doctors supporting me with the same supplements. Please have your hormones checked with saliva or DUTCH testing. Have your complete stool analysis and candida, heli-bacteria, Food sensitivity checked... Because everything starts with the GUT health and main reason for Vagus irritation. I have pocket pills Itake when Afib starts after 2 pm. I take Mag, Taurine Potassium, Q10, multi, probiotics. Enzymes and lately Masticgum heartburn..Incredible positive results for me.....AFIB once a month verses every week, no more burping and gas... Rest of my order same as yours, sleeping position, organic vegetable and juicing...exercise, no whole wheat, gas forming food, no beans... Best of health to everyone, SA.
Reply
joy MacDonald
5/7/2018 09:45:01 am
I too, seem to have vagal AF with episodes that only last for short periods, but I can feel the irregular rhythm when I check my pulse. Mine is definitely triggered when lying on my left side, especially after eating! Therefore I only sleep on my right side and since doing this, I have not experienced the arrhythmia when lying down. Mine is also often precipitated (and treated) by a cough and often I find I need to burp afterwards (I think the gas may actually trigger it). Thank you to all those comments above, very interesting! I plan to try the magnesium and taurine!
Reply
Marilyn Royle
13/7/2018 08:45:39 am
I too am positive I have vagal a fib. I have ongoing problems with my neck and spine after a car accident, which fractured my t6 and had whiplash. I can tell when I’m going into a fib and it’s usually when I slouch, lean over to get something or even stretch up. My posture is really bad these days too. If I eat too much especially after dinner. I have had really bad stomach issues which the gp gave me omeprazole for and also Bisopropol. The omeprazole helped some but the beta blocker did nothing to help in fact I can say it’s made it worse. I have now stopped the beta blocker and am getting attacks more frequently. My gp doesn’t believe it’s vagal related at all, she wants me to wear a heart monitor for a month! At this point I am not taking any medication, i know I will have to soon I’m just not trusting her to give me the correct medication for vagal a-fib.
Reply
Laura Lewis
9/8/2018 11:27:04 pm
Help. On flecainide and inderal and Ativan and Eliquist and go into afib once a week for 9 hours. Take more metoprolol and flecainide to get out of it. So painful
Reply
Grace
12/8/2018 02:45:25 pm
After reading this article and comments, I too, think that I have Vagal Afib. As odd as it sounds, it's exciting to discover this! The other night, after a lovely day in which I had taken good care of myself and avoided known triggers, shortly after lying down in bed - on my back - I could feel the switch flip and the AFib started. My episodes in recent months have been at night or early in the morning if I managed to sleep through the night.
Reply
Kimberly
2/9/2018 07:14:16 am
So glad I found this blog...these symptoms and triggers are all the same for me. I am 49 and it started about 6 years ago. For those with it happening at night...is it possible you are having apena events that are causing it? I have sleep apena and i believe it contributes. I have also hai ed a lot of weight during these years....i cant help think the added pressure on the abdomen triggers the vagus effect.
Reply
Dan
13/9/2018 02:47:39 am
I am 67 years old and discovered I have afib while prepping for a colonoscopy a year ago. I took the polyol purgative overnight and was told at the hospital I couldn't have the test as I was in atrial fibrillation. I was put on metoprolol and losartan and went into CHF after 1 week on medication. I was then put on amiodarone and digoxin in preparation for cardioversion and went into CHF again. Following SOP, I was put back on metoprolol again at a higher dosage titrated in the hospital over 3 days of torture and spun into CHF again for a 3rd time. At this point, I decided to take control of my treatment before the medical community healed me to death. I had an ablation 9 months ago that put me in NSR for 1 month taking diltiazem and fleicanide but the side effects from the fleicanide (my legs turned to concrete) forced me to stop taking it and the afib returned. I know I have vagal afib but I don't have the luxury of triggers as my afib has been 24/7 from its discovery. I've tried Mg, K, taurine, CoQ10, arginine, ribose, carnitine, hawthorne, berberine, acupuncture, etc. to no avail and am at a brick wall. I have no other heart issues and wonder if anyone out there has found a magic bullet to tame the beast?
Reply
Cindy
16/9/2018 05:42:28 pm
All of this is sadly familiar. I have suffered from afib episodes that always occurred at night until one day it happened in the afternoon. I gave up alcohol, and they went back to night time episodes. Without health insurance it was impossible to see a doctor so muddled along as best I could, usually being thankful upon actually waking up in the morning. My episodes have progressed to severe afib episodes that sent me to the emergency room by ambulance. These occur in late evening rather than in the middle of the night. It is the first time seeing anyone for this scary problem. The emergency room physician prescribed a calcium channel blocker, and suggested I see a cardiologist, and after securing health insurance, an appointment was made. He asked me one question twice. Do you take weight loss supplements to which I answered both times, no I do not. He listened to my heart during deep breaths, and then promptly referred me to an endocrinologist. He did schedule an echo cardiogram and also did an EKG, both of which were normal. When I asked his nurse that called with these results what I was supposed to do about the afib she said if it happens again call us and we will do an ablation. This kind of medical treatment, or lack there of has been my experience many times in the past. But I find if I miss a couple days of potassium I have episodes, which also include a lot of peeing. I believe potassium is the root of my problem even though a blood test says it is in the normal range. My magnesium is on the lowest end of normal. It is sad that we are self treating to try to avoid these episodes.
Reply
Russ
20/10/2018 03:03:28 pm
I also have classic vagal afib. Slow resting heart rate, structurally normal heart, attacks always at night, after a big meal, associated w reflux and lying on the L side. Anyone found a Dr or medical center that specializes in this particular problem ?
Reply
Rebecca
24/10/2018 10:07:08 am
I have many of the same triggers mentioned, such as lying on my left side, eating too much or too late, strong emotions, singing, etc. But not mentioned in the article or comments are the effects of electrical fields and other forms of radiation, such as used by smart meters and cell phones. I belong to an electrical hypersensitivity Facebook group and several members, myself included, have arrhythmias and vagus nerve inflammation triggered by exposure to said fields. If I travel to a tech-heavy city or sleep several nights with WiFi on, or stand near a bank of "smart" meters, I will have pronounced changes in my heart rate and rhythms for a week to 10 days afterward. Symptoms vary based on the specific device and length of exposure. For proof that these technologies do indeed affect the heart, please see Magda Havas website (a researcher in Toronto, Canada).
Reply
Jeanne
24/10/2018 05:11:20 pm
This is crazy. I am sure this is what I have. I was at the cardiologist today after a month of a really low heart rate with dizziness followed by waking at 3 am to my heart slowly getting slower, missing a beat, then shaking my entire body like a hiccup when it came back. I went to the bathroom and nearly passed out, with the whole "tunnel vision" thing.
Reply
Lois
28/10/2018 02:56:41 pm
My husband developed afib 3 years ago. After a ton of research, I concluded that that there is likely a link between his afib and his vagus nerve. One promising line of inquiry is explained in this research article on electrical stimulation of the vagus nerve at the site of the ear, called "auricular neuromodulation". https://core.ac.uk/download/pdf/81992462.pdf. This is a pretty new direction with not a lot of research yet on humans. Current research methodology involves using a little TENS-like machine called the Salustim tragus stimulation device. The method apparently has a positive on a number of other conditions as well, including tinnitus and fibromyalgia. I don't know anything else about it at this point, sharing to see if anyone else has heard of or used this technique. Here's another article exploring neuromodulation in a broader way: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5874575/
Reply
Roland alcera
19/6/2019 10:00:22 am
I have my first vagal afib when I was 43, took meds generally for afib that made it worst. Until my cardiologist confirmed it was a vagal one. Taking magnesium citrate really works wonders as I have it under control and was even approved by my cardio. Magnesium citrate is the most easily absorbed and effective type of magnesium.
Reply
Diane Thompson
26/7/2019 12:22:34 pm
Just starting down this A-Fib road. I believe mine to be Vagal A-Fib as well. All the research on related blood clots and strokes has me quite worried. My regular doctor could not hear anything at my last exam so is sending me to a Cardiologist for a Holter Monitor. I definitely feel it after eating, and while laying in bed. The left side seems to trigger and the right side seems to calm it down. So far I have stopped all alcohol, caffeine and started talking magnesium and it seems to have improved. I am anxious to get an answer and start treating it.
Reply
Joy
9/8/2019 06:19:53 pm
I also suffer AF, going on 20 years, 3-5 times a month. HR 150-200, 4-24 hours.
Reply
Margaret Cooke
22/8/2019 04:37:39 pm
Having read the above accounts I believe that I also have vagal induced atrial fibrillation. I am a fit 70 yr old female and only recently started experiencing these cardiac episodes. Rate varies but generally settles within a few hours. Main trigger is lying on left side but have noticed a link with alcohol, sugary bedtime snacks which spike insulin and tea (not coffee). Find it helpful now to unwind with yoga meditation and using a rebounder! My go to supplements for heart health are ubiquinol 150mgs and vitamin B6 alongside L Theanine to support relaxation. Bedtime magnesium 300mgs and taurine 2000mgs have also proved effective in eliminating episodes.
Reply
Gretchen
19/9/2019 07:57:31 pm
How common is this? (Age and sex stratified)
Reply
Bob G
22/9/2019 06:51:56 pm
I am a 45 year old male, pretty good health, non-smoker, healthy lifestyle. Been suffering from afib for over 2 years. When it happens I usually have a pressure below my sternum. Not sure if it's upper stomach or lower diaphragm, but the pressure feels like a fist in the area. Heart rate 150bpm during episodes. Low energy. But, it can stop within a few seconds and be normal 80bpm all of a sudden. Or it can last 18 hours. Anyone have any ideas on how I can get rid of this. Sleeping on left side does seem to be more uncomfortable when I'm in afib. Stress and unhealthy food seems to trigger it sometimes and other times it totally doesn't. Seems so random. My cardiologist wants me to try metropolol 25mg and Multaq (dronedarone) 400mg daily. But I really don't want to take meds. Any help or advice is appreciated!
Reply
Noel
24/9/2019 07:01:16 pm
I am a 72 year old male in reasonably good health who had my first afib episode 13 years ago. My condition is clearly vagal induced, probably by the hiatal hernia I have which causes irritation my esophogus. The problem also causes lung issues, a organ tied into the vagus nerve as well. Many of the causes detailed on this blog apply to me, bad posture, large meals, stomach irritation, sleeping on the left side.
Reply
Ed
10/10/2019 09:11:53 am
I had my first Afib in early 2007 and am writing this in 2019. It was only though reading various posts and articles online that I become aware of the vagal component of my Afib.
Reply
David Kaufman
11/10/2019 02:06:46 am
I am a 61-year old with A Fib since 2006. have previously been diagnosed with vagally mediated A Fib but with no specific treatment for it. I have identical triggers to those presented here and in comments. Tends to start in my sleep. Currently on high dose propafenone + low dose bisoprolol beta blocker. Heart is structurally OK. recently episodes occurring more frequently and for a lot longer duration. Current cardiologist not really interested in my triggers. Is suggesting only real option is ablation and suggests I see an electrophysiologist to discuss it further. I am not sure this is the answer because I have not yet tried some of the complimentary healthcare options mentioned in these comments. Any suggestions?
Reply
Lisa Guillory
26/10/2019 11:40:06 am
I get afib only at night when I lie down, or if I lie down in the evenings. It is definitely made worse by large meals. My heart rate can fluctuate from 48 to 180 in just a few seconds. I usually hold my breath for 15 seconds at a time (like yoga breathing) and it brings the heart rate back down. But even then it often won't convert to normal rhythm, until I sit up or stand up. Last night I slept sitting up and it was the only thing that would keep me in normal rhythm. I refuse to take a rate medication or any medication for this, because I can manage it by breathing techniques but it's disruptive to sleep. It always happens after I lie down. So I can be sleeping normally, get up to go to the bathroom, my heart is in normal rhythm, but when I go back to bed it starts. Last night I dealt with it for 90 minutes until I finally decided to sleep sitting up.
Reply
Tony
30/10/2019 05:12:40 pm
Thankful and relieved to have come across this article and the comments. I'm 36 and have had three episodes of afib in the past 10 years... the most recent one a couple of days ago. Went to the ER/hospital each time. Zapped once... the other two times I converted on my own or chemically (inconclusive). During the episodes, my rate is all over the place for hours... up to 170. Scary and nerve wracking... mind races about heart giving out, blood clots, etc. Doesn't help. I'm otherwise pretty healthy, but should exercise more. Echos and other tests have come back normal. Have PVCs daily/weekly. I share many of the triggers others have shared: big meals, bending over, sleeping on left side, etc. Low potassium levels were cited in the hospital visits. Lack of sleep and stress also seem to be triggers. The biggest trigger for me though is gas in my chest. I have GERD and my esophageal sphincter is basically relaxed/open all of the time. I think maybe gas buildup stimulates the vagus nerve. When I burp (too often), my rhythm/rate feels better. In the most recent episode, I was given Diltiazem and Fleccainide but didn't convert until about 8 hours later. Now considering ablation or pill-in-the-pocket but after reading these comments, thinking maybe I should try Solatol, Magnesium, Taurine, etc. Investigating a gastro solution as well... PPI, hiatal hernia surgery, etc. Anyway, thanks all -- just glad to know I'm not alone.
Reply
Mike
3/11/2019 06:08:12 pm
Thanks everyone for your posts. I feel like this is my exact issue. My story:
Reply
Jon Alchin
5/11/2019 04:23:08 am
I did a search after waking up this morning and getting Afib. I was checking my phone and leaned on my left side for maybe 30 seconds and that triggered it. All of my episodes lately have happened the same way. Left side triggers! I actually feel a little fluttering and if I stand up really quick it stops but I am usually not quick enough and stay in Afib for 30 mins to 3 hours. It always converts on it's own and all the tricks of bearing down or coughing never work for me. I always feeling lethargic after an episode and that lasts all day.
Reply
Yvonne Marshall
12/11/2019 08:05:32 am
I haven't seen any reference to ablation in the discussion here. Is ablation an effective treatment for vagal AFIB? It's interesting that beta-blockers are not a good solution for this type of AFIB. I find that a very low dose of metoprolol seems to have the incidental benefit of helping me with symptoms of anxiety.
Reply
Yvonne Marshall
12/11/2019 08:33:21 am
Oops, regarding my previous comment/question, I just noticed that there is a mention that there is no proven evidence that ablation is effective in treating vagal AFIB.
Reply
Sandra Grinkmeyer
18/11/2019 08:53:39 am
I have many of the symptoms mentioned but one of my differences is that I have a very low heart beat. It can often be 45 or so. I have refused to take Eloquis and instead take a low dose aspirin every night. I also take magnesium and potassium and will now look into Taurine. I have passed out several times during an episode and become quite nauseous -- well first nauseous (always at night/rest or it wakes me up), then vomiting, then passing out. It is very scary and does not happen often. I also suffer from GERD and wonder how much that is involved. I so appreciate all the comments in this article because I also have not gotten much from doctors.
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
Dr Richard BogleThe opinions expressed in this blog are strictly those of the author and should not be construed as the opinion or policy of my employers nor recommendations for your care or anyone else's. Always seek professional guidance instead. Archives
August 2023
Categories
All
|
 RSS Feed
RSS Feed

