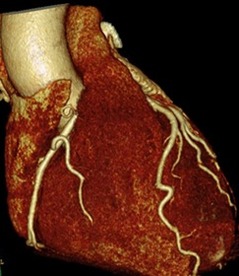
 When you make an initial diagnosis in someone with chest pain, before you do any tests, the chance your diagnosis is correct is called the pre-test probability. As more information comes in from investigations the probability can then be adjusted up or down to decide on further investigation or treatment. An important choice is what investigation to do? In cardiology we have developed a multitude of tests to look for coronary artery disease. We can put our belief in anatomy and do a CT coronary angiogram. his can detect coronary plaque greater than 1mm and has an excellent negative predictive value if it is normal. Alternatively, we could use a physiological test such as exercise ECG, stress echo or nuclear perfusion scans. Depending on where you work, the quality of the local service and your own specialist interests you will make a decision between these different tests. But which is correct? Is it better to use an anatomical or a physiological approach? The PROMISE trial was set up to answer this question. It's a huge trial with 10,003 patients recruited and was published yesterday in the NEJM. They are typical patients just like we see in chest pain clinics. The results are therefore very important for cardiologists. Patients were randomised to either a CT coronary angiogram (4,996 patients) or a physiological test (5,007 patients) with either a stress perfusion scan, stress echo or exercise ECG according to the local preference of the investigators. Patients were followed up for a median of 25 months and the endpoints of the trial were clinical ones including death, non-fatal MI and admission to hospital with unstable angina. An interesting initial result was that the pre-test probability of significant obstructive coronary artery disease was estimated at 53%. In other words 1 in 2 patients were though initially to have significant coronary artery disease. In patients assessed with CT, 12.2% (n=609) were referred on for invasive angiography because significant disease was detected compared with 8.1% (n=406) in the functional testing group. Of the 609 people who had an angiogram after the CT, 28% (170) did not have any significant coronary stenosis and 72% (439) had significant disease. Of the people with significant disease 71% (311) had revascularisation (239 PCI, 72 CABG) and the rest were managed medically. The overall rate of revascularisation from the CT approach was 6.2%. In the functional assessment group 8.1% (n=406) had abnormalities consistent with coronary artery stenosis. Of these 53% (213) had no significant disease on angiography. Of the remained, 193 had coronary artery disease and 82% (158) were offered revascularisation (120 PCI, 38 CABG). The overall rate of revascularisation in this group was 3.2%. So overall in the CT group 8.8% of people investigated had significant coronary stenosis compared to 3.9% in the functional group. So after all the investigation <10% of people had disease compared to the more than 50% suggested by the pre-test probability. This tells us clearly that the models used to assess coronary disease risk which are based on studies done in the 1970s and 80's markedly over-estimate the likelihood of coronary disease. The impression that the risk of coronary disease leads to the high level of investigation which then turns out to be normal in 90% of people. The detection rate for coronary disease by functional testing is about half of that with the CT which then results in half the rate of revascularisation. This is not unexpected since when we assess patients with anatomical tests we tend to overestimate the significance of coronary artery stenosis and this usually leads to a higher rate of revascularisation. Since the primary endpoint of the trial was a clinical one (death, non-fatal myocardial infarction or admission to hospital with unstable angina) and there was no significant difference between the two approaches it seems that either approach is reasonable. But beware if you start with a CT you are 50% more likely to be referred for an invasive angiogram and after that twice as likely to be offered revascularisation with no significant difference in clinical event rates. This of course has cost implications. If we assume that the anatomical and function testing is of similar cost initially but CT leads to more angiography and revascularisation then using some simple tariff costs the CT approach in the end costs almost twice as much. An interesting point to ponder for CCGs who might want us to use CT as the first line investigation in the belief that it reduces the need for invasive angiography.
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
Dr Richard BogleThe opinions expressed in this blog are strictly those of the author and should not be construed as the opinion or policy of my employers nor recommendations for your care or anyone else's. Always seek professional guidance instead. Archives
August 2023
Categories
All
|
 RSS Feed
RSS Feed

